USU Dermatology Offers Steps to Take for Skin Cancer Detection and Prevention
By Ensign Claire Sturek, U.S. Navy and Col. (Dr.) Sunghun Cho, U.S. Army
The return of warm weather and sunny skies in May mark more than the start of tank top season. May is skin cancer awareness month, and is an opportunity to increase the community’s knowledge about skin cancer and sun protection.
One in five Americans is diagnosed with skin cancer during their lifetime, making this the most common form of cancer in the United States. About 95% of these are non-melanoma cancers, and the majority of these are basal cell carcinomas (BCC) and squamous cell carcinomas (SCC). Melanomas are the deadliest form of skin cancer and have a higher chance of spreading internally. All skin cancers have an extremely high cure rate if detected and treated early. Nonetheless, invasive SCC and melanomas account for over 20,000 lives lost each year in the United States. Although skin cancers may be less prevalent in skin tones with more pigment, they can go undetected for longer and present at advanced stages.
Not surprisingly, the risk of skin cancer is higher for those with outdoor occupations, including members of the Armed Forces. All forms of skin cancer are strongly associated with ultraviolet (UV) radiation exposure, namely ultraviolet A (UVA) and ultraviolet B (UVB). UVA rays additionally cause premature aging such as wrinkling and age spots. This form of UV radiation can penetrate window glass, exposing you even when indoors or inside your car. UVB rays are the sun’s burning rays and while they are blocked by window glass, they play the greatest role in causing skin cancers. The World Health Organization International Agency for Research on Cancer has emphasized this link by identifying solar UV radiation and UV tanning devices as carcinogens. The incidence of skin cancer is predicted to increase in our Active Duty and Veteran populations due to high UV radiation exposure during recent engagements in the Middle East, further highlighting the importance of skin cancer awareness, education, and prevention efforts in our community.
Prevention
While there are non-modifiable genetic risk factors for skin cancers, exposure to UV radiation can be controlled by using a combination of sunscreen, protective clothing, and seeking shade when the sun’s rays are strongest between 10 a.m. and 4 p.m.
When selecting a sunscreen, look for a water-resistant sunscreen with a Sun Protection Factor (SPF) of at least 30. SPF refers to the product’s ability to provide UVB protection, which helps prevent sunburn. The higher the SPF, the more UVB protection, but the level of protection does not increase proportionately. SPF of 30 blocks about 97 percent of radiation, and SPF 50 blocks 98 percent of UVB rays. Ensure that your sunscreen is broad-spectrum, indicating both UVA and UVB coverage. Sunscreen should be applied to all exposed skin 20 minutes before going outdoors and rubbed in thoroughly. Most people apply only 20 to 50 percent of the recommended amount of sunscreen. One ounce, enough to fill a shot glass, is the typical amount of sunscreen needed to cover the exposed areas of the body evenly. When applied once every two hours, sunscreens offer excellent protection.
In general, clothing with long sleeves, long pants, and wide brimmed hats provide adequate coverage. When shopping for protective clothing, a fabric’s ultraviolet protection factor (UPF) rating can be a helpful tool. It is analogous to sun protection factor (SPF), and higher numbers provide additional protection.
Detection
Skin cancers are very treatable and have excellent outcomes when detected early. You can take charge of your health by checking your skin regularly. Although sun-exposed skin on the face, hands, neck, and arms are the more common places to develop skin cancer, any surface is susceptible. In particular, skin cancers in more pigmented skin tones often present on hands, feet, lower extremities, and non-sun exposed areas of skin. It is important to examine the entirety of the skin including along the nails, scalp, and genital regions for suspicious growths. Having a partner examine hard to see areas, like the back, can be very helpful.
When performing skin checks, be on the look-out for new growths that do not go away on their own. Lesions suspicious for skin cancer may be dark, bleed, change rapidly, or heal poorly. They may also exhibit the ‘ugly duckling sign,’ appearing out of place when compared to other growths on the body.
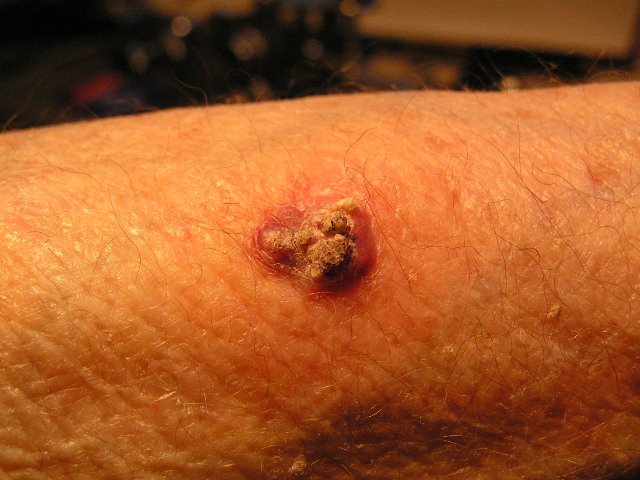 |
Figure 2: Squamous Cell Carcinoma on the arm presenting as a thickened papule |
.jpg) |
Figure 3: Basal Cell Carcinoma on the nose with telangiectasias and rolled borders |
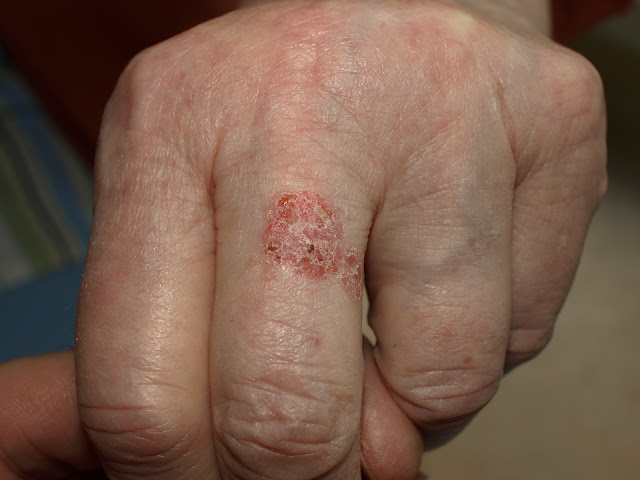 |
Figure 4: Non-melanoma skin cancer can masquerade as a rash that does not heal |
Final Thoughts
Skin cancer is a common, yet highly preventable and treatable condition. Taking adequate measures to protect skin from UV exposure, performing regular self-checks, and having a low threshold for contacting your health care provider can provide the best health outcomes, especially within our high-risk community. We encourage you to practice good UV hygiene starting this month and throughout the rest of the year!
References:
Riemenschneider, Kelsie, et al. “Skin Cancer in the Military: A Systematic Review of Melanoma and Nonmelanoma Skin Cancer Incidence, Prevention, and Screening among Active Duty and Veteran Personnel.” Journal of the American Academy of Dermatology, June 2018, https://doi.org/10.1016/J.JAAD.2017.11.062.
Stubblefield, Jonathan, and Brent Kelly. “Melanoma in Non-Caucasian Populations.” Surgical Clinics of North America, vol. 94, no. 5, 2014, p. Pages 1115-1126, www.sciencedirect.com/science/article/pii/S0039610914001078, https://doi.org/10.1016/j.suc.2014.07.008.. Accessed 10 May 2022.
Skin Cancer Foundation. (2022 Jan). Skin Cancer Facts and Statistics. Skincancer.org. https://www.skincancer.org/skin-cancer-information/skin-cancer-facts/

.jpg)



